A patient we’ll call Janet contacted our clinic in a state of distress. What began as a seemingly benign bruise a day after her chin and jawline filler injections spread to her cheek and forehead. Subsequently, her eyelids became bruised and edematous, and purple marks appeared on her temple, tracing the path of her arteries. When she sought help from the clinic that administered the injections, the doctor was unavailable. It took days before she was finally diagnosed with vascular occlusion and began treatment, which included hyperbaric oxygen therapy, aspirin, hyaluronidase injections, and even Viagra to improve blood flow. Yet, the sinister purple marks continued to spread, and the areas remained exquisitely painful. With a growing sense of alarm, she reached out to our office.
In aesthetic medicine, few situations are true emergencies. Even with vascular occlusion, like in Janet’s case, there’s typically a treatment window of 2–3 days. However, by the time Janet reached us, that critical period had elapsed, and we found ourselves in a race against time to prevent ischemic tissue damage. Fortunately, our clinic is well equipped for such emergencies, armed with a high-resolution ultrasound device and years of experience.
Filler-related vascular occlusion, with the pain of ischemia, and subsequent treatments, along with the looming threat of facial necrosis and the anxiety over uncertain outcomes, can be a daunting experience for both practitioners and patients. In these situations, ultrasound becomes invaluable. Its ability to provide real-time visualization of affected vessels and the occlusive filler enables precise, ultrasound-guided hyaluronidase injections that dissolve the filler, improve arterial spasm, and restore blood flow. Once the occlusion is treated, Color Doppler can demonstrate immediate improvement in blood flow, correlating with clinical recovery and providing reassurance to both patients and medical practitioners.
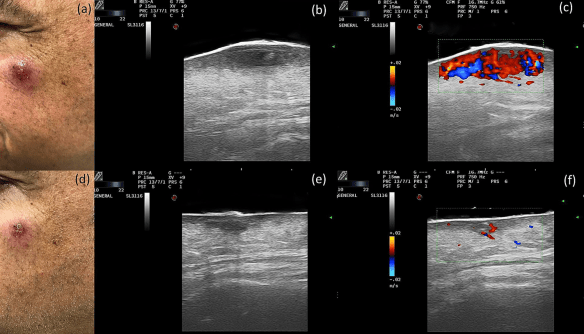
Janet’s ultrasound exam revealed several areas of blockage along the facial arteries, with adjacent filler deposits. We found areas of decreased blood flow along the jaw, in her cheek, in the temple, and at the mandibular angle, with large deposits of anechoic hyaluronic acid filler adjacent to them. We also discovered and treated severely decreased flow in the facial vein, which likely explained the unusual periorbital edema and ecchymosis. You can see one area of compromised blood flow in Figure 1.
We treated these areas with ultrasound-guided hyaluronidase injections, as depicted in Figure 2.
By the following day, Janet’s condition had shown marked improvement, and the pain had subsided. Improved blood flow in both the facial artery and facial vein can be seen in Figure 3.
Over the last several years, we have witnessed an exponential increase in the number of aesthetic treatments. However, as we keep pushing the envelope to improve our patients’ results and the longevity of our treatments, we face a growing number of complications, including overfilled faces, filler malposition and migration, lumps, chronic edema, and vascular complications such as vascular occlusion, and even stroke and blindness. Vascular occlusion, one of the most dreaded filler complications, has been the main impetus behind the introduction of ultrasound into aesthetic medicine.
This process could not have come at a better time. The use of ultrasound offers a blend of opportunities and challenges that are reshaping our profession. From mastering facial anatomy and adopting safer injection techniques to managing complications more effectively, aesthetic practitioners can harness the power of ultrasound to advance their practice and patient care, refine techniques, enhance safety, and improve patient outcomes.
References:
- Desyatnikova S, Schelke L. Treatment of filler-related vascular occlusion using handheld portable ultrasound device. J Cosmet Dermatol 2022; 21:3166–3168. doi: 10.1111/jocd.15125.
- Desyatnikova S, Barrera P. High-resolution ultrasound for diagnosis and treatment of filler-related septal necrosis. Plast Reconstr Surg Glob Open 2024; 12:e5630. doi: 10.1097/GOX.0000000000005630.
- Choi SY, Shin SH, Seok J, Yoo KH, Kim BJ. Management strategies for vascular complications in hyaluronic acid filler injections: A case series analysis. J Cosmet Dermatol 2023; 22:3261–3267. doi: 10.1111/jocd.15990.
- Schelke LW, Velthuis P, Kadouch J, Swift A. Early ultrasound for diagnosis and treatment of vascular adverse events with hyaluronic acid fillers. J Am Acad Dermatol 2023; 88:79–85. doi: 10.1016/j.jaad.2019.07.032.
Stella Desyatnikova, MD, is a double board-certified facial plastic surgeon, with over 20 years’ experience. She is the founder of The Stella Center for Facial Plastic Surgery and the Ultrasonos Aesthetic Ultrasound Training Center in Seattle, WA. She is a leading authority in aesthetic ultrasound research and education, committed to expanding education and awareness of ultrasound use to optimize safety of aesthetic procedures. Her research is focused on filler injectable safety and facial ultrasound applications. She is the Secretary-elect of the Dermatology Community of the American Institute of Ultrasound in Medicine (AIUM). She is also an International Expert Board Member of the Complications in Medical Aesthetics Cooperative (CMAC) and a member of the American Academy of Facial Plastic and Reconstructive Surgery (AAFPRS).
Interested in learning more? Check out the online Advanced Dermatologic Ultrasound Course on September 7–8, 2024, with renowned faculty including Stella Desyatnikova, MD.













 I saw a “hockey stick” probe. Instinctively, I decided to use it on my fingernails. The images I saw on the screen were so fantastic that I ran to the library to see if there were any papers or publications that focused on ultrasound of the nail.
I saw a “hockey stick” probe. Instinctively, I decided to use it on my fingernails. The images I saw on the screen were so fantastic that I ran to the library to see if there were any papers or publications that focused on ultrasound of the nail.