I trained as a physiatrist, which means a great deal of education on musculoskeletal conditions. Over the course of my residency training, I became more and more comfortable with bony and soft tissue landmarks for examination and targeting various joints, nerves, and tendons for therapeutic injections. As I was supervised by attendings, and carefully followed their instructions, there was no doubt in my mind that the tip of my needle was at the target intended. Why would I doubt a common practice that has been in existence for several decades?
As I started my fellowship in spine/pain/musculoskeletal care, I found the love of my life, the fluoroscope!! Here, I had access to a tool that made life incredibly easy. I actually could visualize my targeted hip, shoulder, or facet joint, and inject some contrast to identify the needle tip within my target. I could precisely deliver therapeutic medications to a particular nerve root, and even identify vascular uptake and avoid procedural complications.
It was then and there that I realized that there were substantial shortcomings in what I learned as “landmark-based injections”. I realized that even though I had learned the proper “blind” procedure technique, there was no confirmation that my medication had reached its intended target. More importantly, if my patient did not respond to the procedure, I could not differentiate between a medical condition that was not responsive to the treatment versus shortcomings of un-guided procedures and inadequate delivery of medications to the targeted tissue/joint. For 12 years, I confidently treated thousands of patients by performing spine and musculoskeletal injections using my fluoroscope. I enjoyed using my C-arm, and life was pretty good.
In 2011, while attending a PM&R national conference, I sat through a 15-minute presentation on overdiagnosis of trochanteric bursitis. The speaker eloquently described fluoroscopic-guided bursa injection. This was something that I did on a regular basis as a diagnostic step. He then used ultrasound (US) images to demonstrate a few cases of gluteus medius tendinopathy and also trochanteric bursitis and how US can be superior to X-ray in therapeutic sub-gluteus maximus bursa injection. While sitting and listening, I recognized that it was virtually impossible to press against the lateral trochanter and be accurate about the diagnosis. It is also not possible to use fluoroscopy and be sure that the steroid or regenerative treatments are correctly delivered to sub-gluteus maximus bursa.
Remembering how helpful fluoroscope was to identify particular bony landmarks and assist with the proper treatment of spine and joint disease, here I was discovering a new tool that can enhance diagnostic and therapeutic skills in musculoskeletal care in particular soft tissue disease (nerves, muscles, tendons). This meant a fundamental change in the way I was going to treat patients but also a change in how I train the next generations of Physiatrists, coming through our residency program.


Learning to use the US, and incorporating it into the practice was much harder than I envisioned and also very expensive. At the time, there were limited well-structured educational resources available, and the learning curve was quite steep. As I was learning, I had to beg (or pay) my kids to become my scanning subjects!!
In contrast to a fluoroscope, it is nearly impossible to recognize an abnormal structure on the US unless you are comfortable with the normal anatomy. With a ton of hands-on workshops, mentorship, practice, and with assistance from my new found love of ultrasound machine, and guidelines from the AIUM, ultrasound has become easier and more enjoyable!! The abnormal findings became more clear and treatments more effective. In this process, I found out that patients enjoy looking at the US screen and being explained about finding on a screen full of gray, gray, and grayer lines and curves.
US has transformed how physiatrists practice and teach musculoskeletal medicine. Point-of-care US imaging allows for the residents and fellows to visualize various organs or structures within an organ, recognize healthy and diseased tissue, and diagnose the problem on the spot. This, in turn, will lead to a quick and targeted treatment and satisfied patients.
Examples of musculoskeletal (MSK) conditions that US has proven to be an effective tool to workup or treat includes rotator cuff and biceps tendinopathy, small or large joint injections, upper extremity nerve entrapments, muscle and tendon tears, peripheral nerve lesions, carpal tunnel syndrome (CTS), intersection syndromes, trigger fingers, plantar fasciitis, piriformis and sciatic complaints, treatments of bursitis or tenosynovitis, iliotibial (IT) band treatment, ischiofemoral impingement, and many diagnoses for which dynamic testing proves to be beneficial.

Despite its cost and extensive training/certification needs, utilization of US in MSK care is predicted to be a standard of care in the next 5–10 years. As more and more practitioners are trained, its use for diagnostic or therapeutic purposes will become the norm.
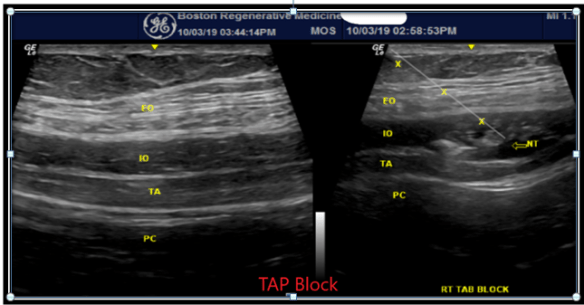

I still love my fluoroscope and prefer its use in most spine procedures. Adding US has revolutionized my practice and allows me to be a better diagnostician, a better MSK doctor and a better educator for both my patients as well as future providers that come after me. In short, US has been a game-changer.
Ali Mostoufi, MD, FAAPMR, FAAPM, is an Assistant Prof. in PM&R at Tufts University, and the president of New England Spine Care Associates (NeSpineCare.com) and Boston Regenerative Medicine (BostonRegen.com). As a spine and sports medicine practitioner, his clinical practice focuses on Interventional Spine, Diagnostic US, US-based therapeutic interventions and Regenerative Medicine in spine and sports.
Interested in reading more about musculoskeletal ultrasound? Check out the following posts from the Scan:
- Ultrasound-Guided Musculoskeletal Injections by Bryant Walrod, MD, CAQSM
- A Future Career Path for the MSK Sonographer by Alan Solomon, MD
- Ultrasound Set to Transform Occupational Medicine by Yusef Sayeed, MD, MPH, MEng, CPH
- Interdisciplinary Education and Training in MSK Ultrasound by Yusef Sayeed, MD, MPH, MEng, CPH
- A Major Boon for Physical Therapy by Colin Thomas Rigney, PT, DPT, OCS, RMSK
Comment below, or, AIUM members, continue the conversation on Connect, the AIUM’s online community to share your experience.














Thanks for Sharing This Article. It is very so much valuable content. I hope these Commenting lists will help to my website. Thanks for sharing such good stuff with us.
Hi friends,
Nice idea, keep sharing your ideas with us. i hope this information will be helpful for the new learners. I have no words for say really amazing article.